
level-headed
“Every living thing wants most of all to live. And I am no different.”

It’s 6:30 a.m. on a Saturday morning and I hear the patpatpat of children’s feet rattling the hardwood floor above me. The giggles and feet of two young boys hit the top of the staircase until the familiar voice rings, “Brush your teeth before going downstairs!” There is a pause, then, ‘Yes, Mom,” with the ‘Mom’ drawn out, poorly masking their indignation.
Luca Cantua, the 11-year-old perfectionist and elder brother to Parker, heads to the kitchen and signals with sleepy eyes for a hug and kiss from his mother, Holly Cantua. After their morning embrace, the two perform their daily dance. Luca waltzes to the refrigerator, finding his favorite flavored Go-Gurt. Holly glides to the sink, sweeping up a bottle of medication. The two then join, exchanging bowls, opening capsules, and pouring the dust of medication into the overly-sweet yogurt.
Two years ago, Luca was diagnosed with epilepsy, a chronic brain disorder resulting in recurring seizures. For Luca in particular, his seizures consist of staring spells, with flickering eyelids and a loss of consciousness. His seizures are controlled by medication as long as he takes it at the same time each day, morning and night. Though he has been seizure-free for over one year, each member of his family is on edge, prepared for one to occur at any time.

After his morning dose of Depakote, Luca takes his daily shower with the door slightly ajar, either Mom or Dad asking, “Everything okay?” until they hear the water shut off. This phrase is repeated quite often in the Cantua household. Whether Luca is staring out the window on a long car ride, taking a shower or watching television, he’ll be prompted with an “Everything okay?” that is often followed by a slightly-defiant “Yes, why are you asking?”

Luca describes a feeling of deep frustration with his parents’ concern because he wants to be treated “normally.” At the same time, he feels exasperated when he experiences side effects from his medication or a seizure (exhaustion, confusion, or emotional stress), because the people around him cannot see the pain he endures. Because Luca looks healthy, he must constantly explain, in detail, his pain (and hope the person believes him). Some days, he does not have the energy to translate his brain’s defaults. He pushes through the pain and finishes the school day or does the extra lap on the soccer field.

The dichotomy between the desire for complete normalcy while simultaneously being accommodated to is a common experience for those diagnosed with a health condition early in life. Luca describes this complex situation with one emotion: loneliness. Luca’s emotional distress roots from the yearning for a normal life while attempting to come to terms with his reality. He says knowing more people with epilepsy, people who “know what it’s like,” is what he truly wants. Luca’s search for identity is muddled by the belief that he “is the only person like this.”
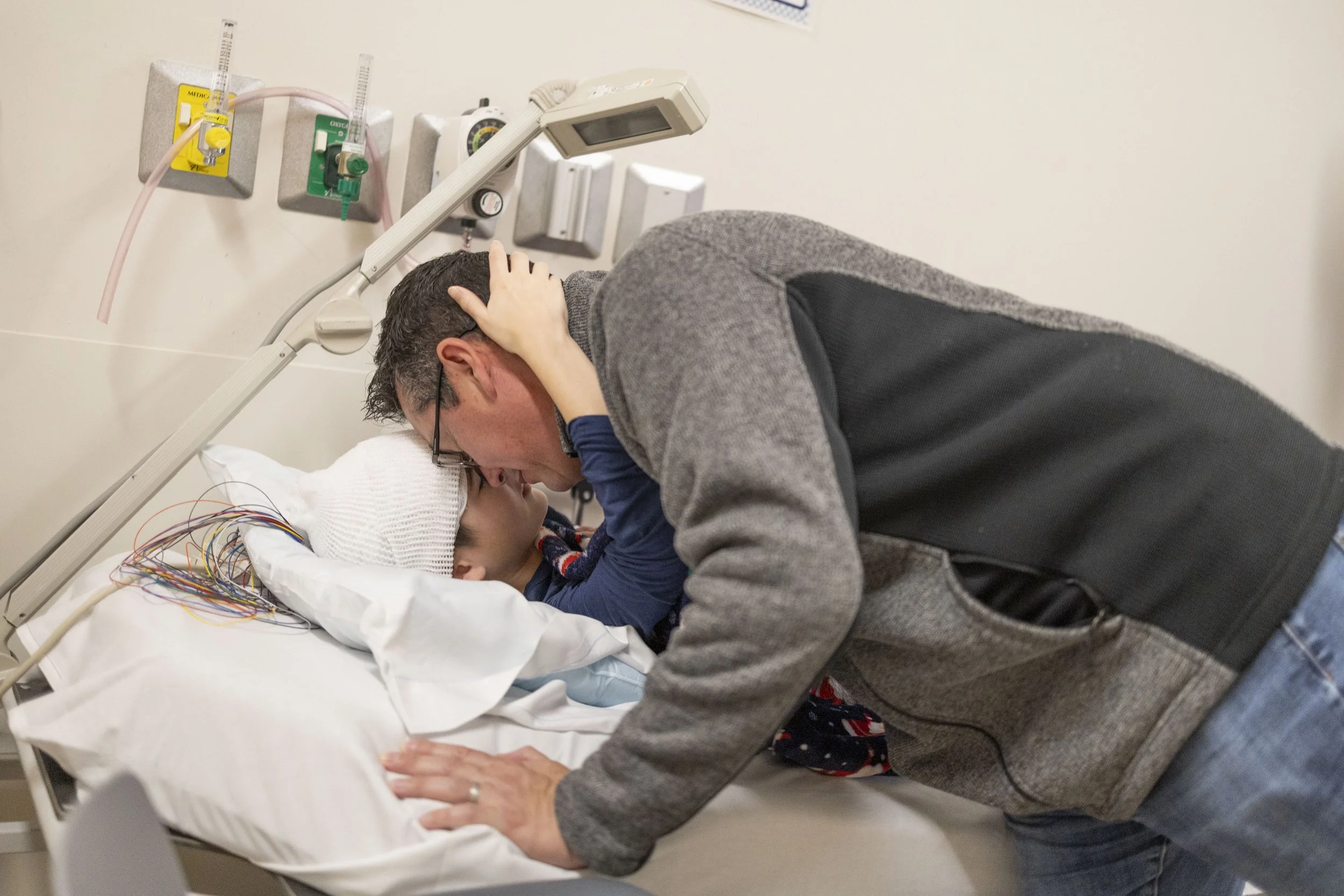
Because Luca only has discussions about epilepsy with his doctor or telling people what to do in case of a seizure, he has not yet explored what it means to him. Luca longs to learn more about his condition and seeks outside knowledge through Youtube videos, online research and other colder, factual outlets of learning about himself because he does not know anybody who has the answers he is searching for. He is hungry for answers of what epilepsy means to him and how to cope with it.
“I feel kind of annoyed when everyone is asking about my seizures,” says Luca. “But if they don’t ask questions, I feel like they don’t care about me… It’s kind of confusing. It would be cool to have a friend that is also confused and we can talk about that.”
Luca’s experience is not uncommon. 1/26 people have epilepsy, yet most people diagnosed report never having met another person with the condition. People with epilepsy, and many other conditions, often hold back from speaking on their maladies due to a sense of shame for not being “normal.” As a result, most people with “invisible” conditions often experience isolation.
Because people with epilepsy refrain from speaking out against their experiences, there is a misconception of the prevalence of the disability. Epilepsy is the third-most common neurological disorder, yet receives 10 times less funding than any other brain disorder. It impacts more people than Alzheimer’s disease, multiple sclerosis and Parkinson’s disease combined, yet most people aren’t aware of what epilepsy means and how it affects those diagnosed.
In order to increase funding for an illness or disability, it is necessary to have a strong community advocating for those diagnosed. If those afflicted with epilepsy had a larger platform to speak on their experiences with neurologists, medications, etc., there is potential for significant changes to the medical care that epilepsy patients receive.
Because the cause of epilepsy is still unknown, greater funding in research has the ability to crack a code in how patients are treated. Current researchers have made significant progress, with 70% of people diagnosed with epilepsy in the United States having controlled seizures. With increased funding and improved research, all diagnosed with epilepsy have the potential to be seizure free.


When Luca grows up, he wants to be a neurologist that treats people with epilepsy. By that time, he hopes that there is a cure and that he can give it to his patients. He wants to foster an epilepsy community one-by-one. Luca can serve as an inspiration to those with a health condition – to always search for and help those who may be going through the same afflictions that you are.

Considering these impacts, one can see community as a vessel for greater change for epilepsy care and in the public health field as a whole. An audience is more likely to listen to a large group of individuals afflicted with a condition rather than just one.
When Luca speaks of his feelings of loneliness, he does not speak of them with finality. Instead, he speaks of his experience as something temporary. He says he feels alone “right now.” When asked what he sees for his future, he often says that he knows that a lot of people in the world have epilepsy, and he knows he will one day become friends with one of them.

“I want to help make people with epilepsy better because I care about everyone with epilepsy,” says Luca. “Even if I don’t know them, they are my friends. It feels good to know that I have so many friends. Even though I haven’t met them yet.”
1/26 people living in the united states have epilepsy❋ Funding inequity
Epilepsy is the fourth most common neurological disease and the least funded. It receives 7.7x less funding than Alzheimer's (#3) and 1.4x less than stroke (#1), a condition that can leave people living with epilepsy in its aftermath.
❋ Treatment Disparities
Higher rates of poverty are linked to increased epilepsy incidence, lower medication adherence, and reduced access to care. Up to 75% of people with epilepsy in low-income countries going untreated.
❋ Access to care
African American and Hispanic individuals are less likely to see an outpatient neurologist or access specialized epilepsy centers, often relying on emergency care. Implicit bias in healthcare settings can result in lower quality care, fewer diagnostic tests (like MRI or EEG) being ordered, and less likelihood of being referred for epilepsy surgery.
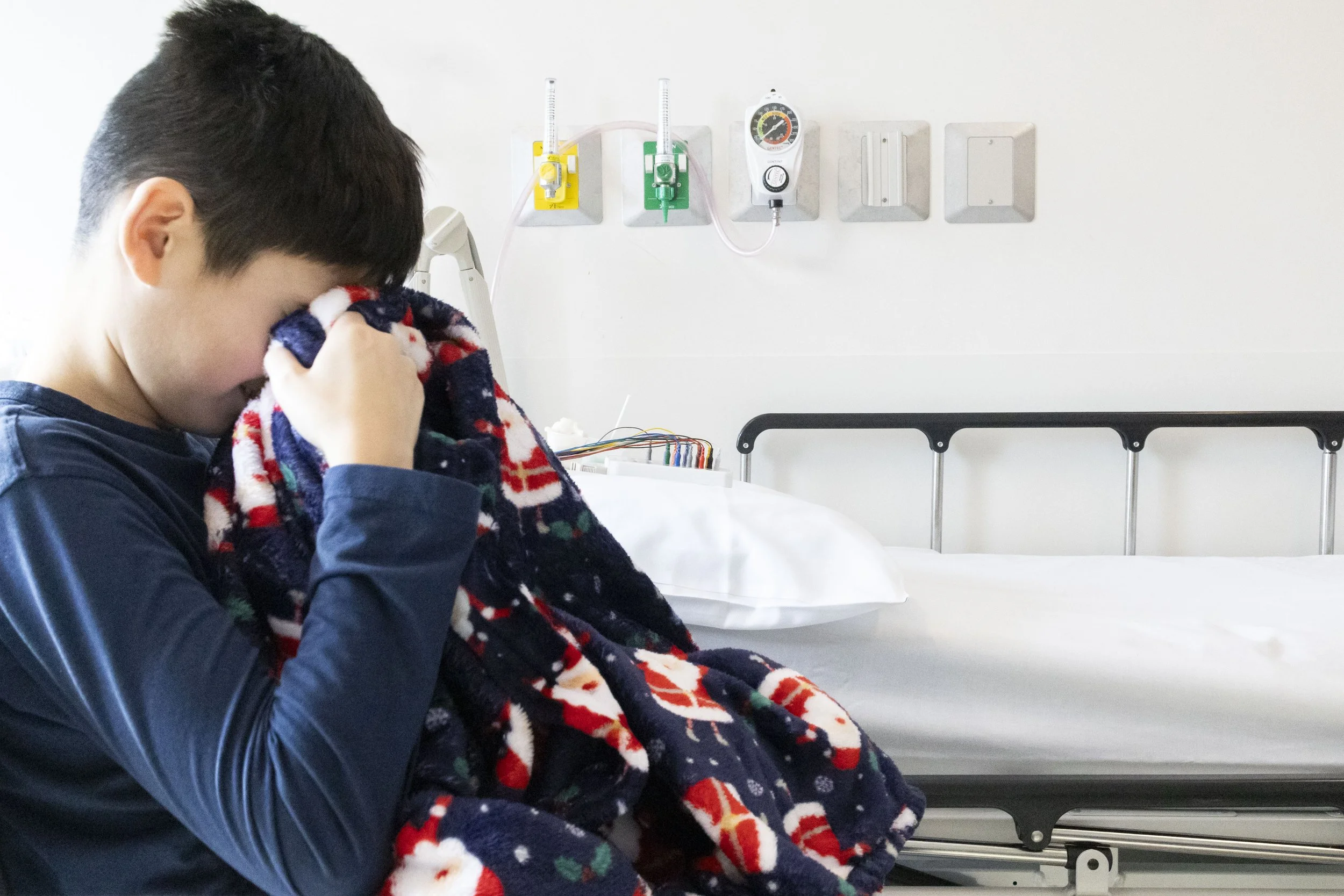


How Can I support the cause?
Join us in the Walk for Epilepsy hosted by tallulah Brown Van Zee and the Epilepsy Foundation
on May 2, 2026 at Sandy Point State Park
